Introduction
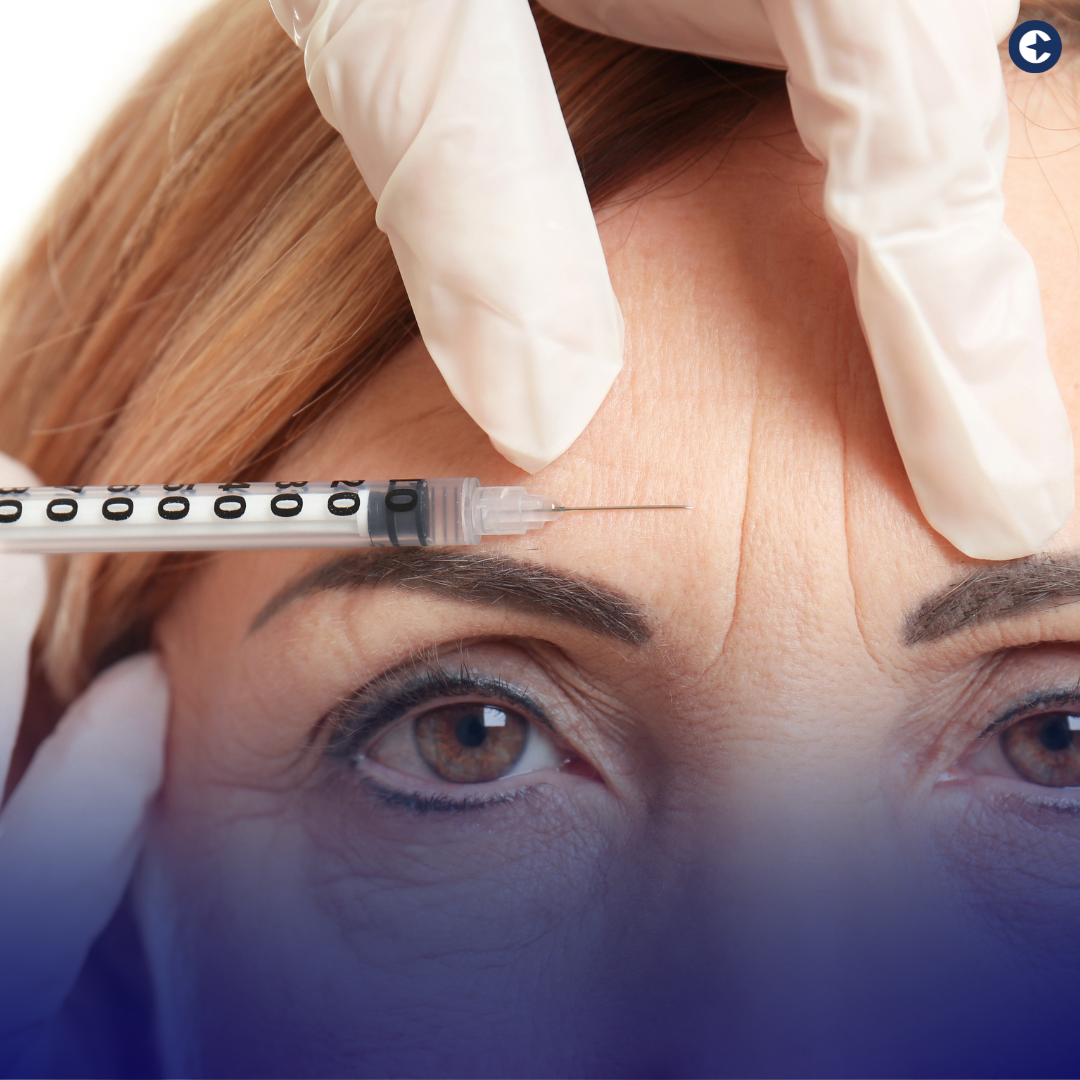
Botox, a name synonymous with cosmetic procedures for reducing wrinkles and fine lines, has steadily gained popularity worldwide. However, its uses extend far beyond cosmetic enhancements. As we celebrate Botox Day, it’s essential to delve into the broader spectrum of Botox applications and understand the nuances of insurance coverage for this treatment.
The Multifaceted World of Botox
Traditionally, Botox is known for its ability to smooth out wrinkles, offering a more youthful appearance. However, its therapeutic applications are equally noteworthy. Botox, or Botulinum toxin, is used for various medical conditions, including chronic migraine, excessive sweating (hyperhidrosis), muscle spasticity, and certain eye disorders.
Insurance Coverage for Botox: A Complex Landscape
The coverage of Botox by insurance companies largely depends on the purpose of the treatment:
- Cosmetic vs. Medical Necessity: Insurance typically covers Botox treatments when deemed medically necessary. For example, patients with chronic migraines may receive coverage for Botox injections as a form of preventive treatment. Similarly, those suffering from conditions like hyperhidrosis or blepharospasm (eyelid spasms) may also be eligible for insurance benefits.
- Policy Specifics: It’s crucial to understand your health insurance policy. Coverage can vary widely between different insurers and plans. Some may cover a portion of the cost, while others might require specific criteria to be met before approving coverage.
- Documentation and Diagnosis: For insurance to cover Botox treatments, a clear medical diagnosis from a healthcare professional is often required. This diagnosis must justify the use of Botox as a necessary treatment for the condition.

Cosmetic Botox and Insurance
When it comes to cosmetic applications, such as anti-aging treatments, insurance typically does not provide coverage. These procedures are considered elective and non-essential from a medical standpoint. Patients opting for Botox for cosmetic reasons should be prepared to cover the full cost out-of-pocket.
Navigating Insurance Claims for Botox
If you’re considering Botox for a medical condition, here are some steps to navigate the insurance process:
- Consultation with a Healthcare Provider: Discuss your condition and treatment options with a qualified healthcare professional.
- Insurance Verification: Contact your insurance provider to verify coverage and understand any prerequisites for claims.
- Documentation: Ensure your healthcare provider documents your condition and the necessity for Botox treatment.
- Follow-up: Keep track of your treatment and maintain communication with both your healthcare provider and insurance company.
Conclusion
Botox Day not only celebrates the cosmetic benefits of this versatile treatment but also sheds light on its significant medical applications. Understanding the distinctions between cosmetic and medical use is crucial for navigating insurance coverage. Always consult with healthcare professionals and your insurance provider to make informed decisions about Botox treatments.
Note: This blog provides general information and should not be considered medical advice. Always consult with healthcare professionals for medical concerns and insurance experts for coverage-related questions.
For more follow us on Instagram, Facebook, Twitter, & LinkedIn.